Complex Neurology Care
Dr. Zuber and his team of professionals will guide you through your diagnosis and treatment process, ensuring you receive the high quality care you deserve.
Patient Resources
We have our intake forms conveniently stored online and can be printed in the privacy of your own home.
Get In Touch
We're only a simple click or phone call away. You have a team that is here to listen, help and care for your needs.
Conditions we treat
- ALS (Lou Gehrig’s Disease)
- Alzheimer’s Disease
- Ataxia (Gait disorders)
- Bell’s Palsy
- Brain Aneurysm
- Brain Concussion
- Brain Injury
- Carpal Tunnel Syndrome
- Cerebral Artery Thrombosis
- Cerebral Vascular Disease
- Cervical Radiculopathy
- Chiari’s Deformity
- Chronic Fatigue Syndrome
- Convulsions
- Cranial Trauma
- Dementia
- Diabetic Polyneuropathy
- Diplopia
- Dizziness and Imbalance
- Dystonia
- Epilepsy
- Essential Tremor
- Excessive Daytime Somnolence
- Fainting and Near Fainting
- Fibromyalgia
- Gait and Balance Disorders
- Giant Cell Arteritis
- Headaches
- Huntington’s Disease
- Hydrocephalus
- Inflammatory Toxic Neuropathy
- Insomnia
- Intervertebral Disc Herniation
- Low Back Pain
- Memory Problems
- Meningiomas
- Migraines
- Multiple Sclerosis (MS)
- Muscle Spasms and Cramps
- Muscle Weakness
- Myasthenia Gravis
- Myoclonus
- Narcolepsy
- Neurological Malignancies
- Neuropsychiatric disorders
- Numbness and weakness
- Normal Pressure Hydrocephalus
- Numbness and/or Tingling
- Optic Neuritis
- Parkinson’s Disease
- Peripheral Nerve Disorders
- Pseudotumor Cerebri
- Radiculopathy
- Restless Leg Syndrome
- Seizure
- Sleep Apnea
- Spina Bifida
- Spinal Stenosis
- Stroke and TIA
- Syncope
- Tic disorders
- Transient Ischemic Attack (TIA)
- Tremors/Shaking
- Trigeminal Neuralgia
- Tuberous Sclerosis
- Vertigo and Dizziness
- Visual Field Defects
DIAGNOSTIC TESTING
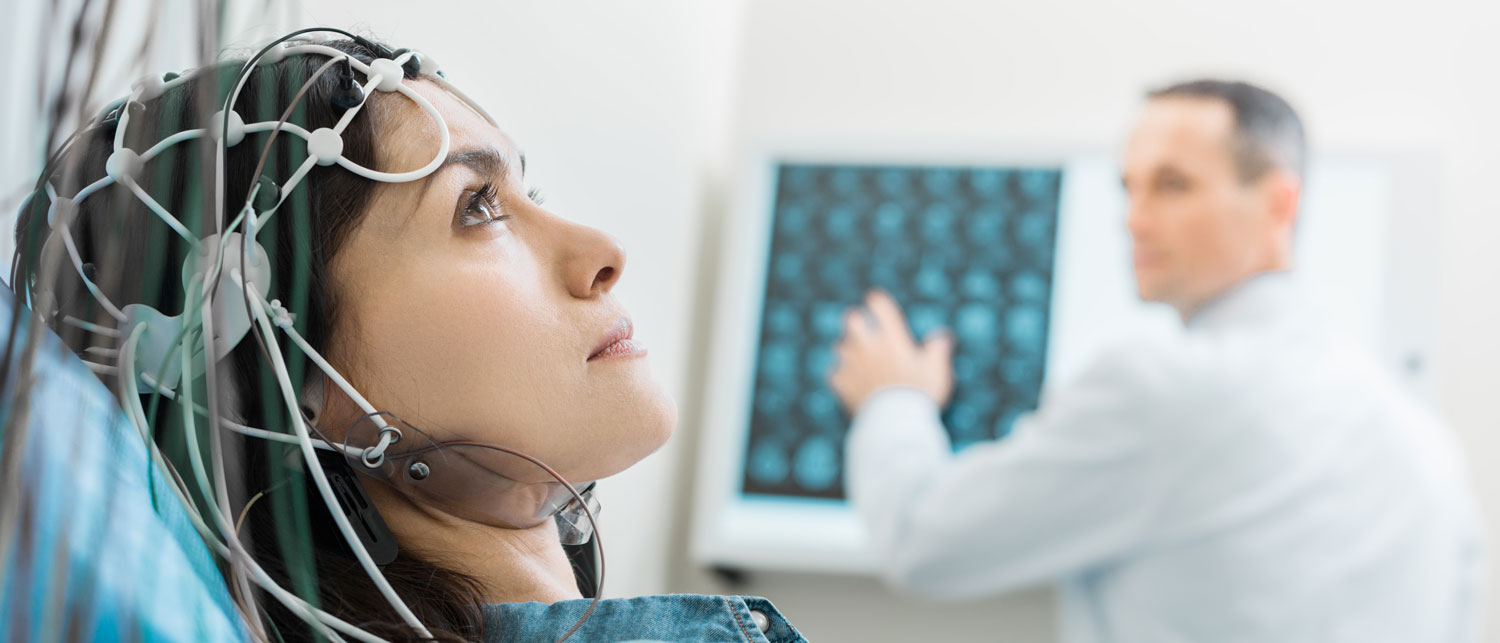
Electroencephalography (EEG) is an electrophysiological monitoring method to record electrical activity of the brain. It is typically noninvasive, with the electrodes placed along the scalp, although invasive electrodes are sometimes used, as in electrocorticography. EEG measures voltage fluctuations resulting from ionic current within the neurons of the brain. Clinically, EEG refers to the recording of the brain’s spontaneous electrical activity over a period of time, as recorded from multiple electrodes placed on the scalp. Diagnostic applications generally focus either on event-related potentials or on the spectral content of EEG. The former investigates potential fluctuations time locked to an event, such as ‘stimulus onset’ or ‘button press’. The latter analyses the type of neural oscillations (popularly called “brain waves”) that can be observed in EEG signals in the frequency domain.
EEG is most often used to diagnose epilepsy, which causes abnormalities in EEG readings. It is also used to diagnose sleep disorders, depth of anesthesia, coma, encephalopathies, and brain death. EEG used to be a first-line method of diagnosis for tumors, stroke and other focal brain disorders, but this use has decreased with the advent of high-resolution anatomical imaging techniques such as magnetic resonance imaging (MRI) and computed tomography (CT). Despite limited spatial resolution, EEG continues to be a valuable tool for research and diagnosis. It is one of the few mobile techniques available and offers millisecond-range temporal resolution which is not possible with CT, PET or MRI.
Derivatives of the EEG technique include evoked potentials (EP), which involves averaging the EEG activity time-locked to the presentation of a stimulus of some sort (visual, somatosensory, or auditory). Event-related potentials (ERPs) refer to averaged EEG responses that are time-locked to more complex processing of stimuli; this technique is used in cognitive science, cognitive psychology, and psychophysiological research.
Electromyography (EMG) Nerve Conduction Study (NCS) is an electrodiagnostic medicine technique for evaluating and recording the electrical activity produced by skeletal muscl EMG is performed using an instrument called an electromyograph to produce a record called an electromyogram. An electromyograph detects the electric potential generated by muscle cells when these cells are electrically or neurologically activated. The signals can be analyzed to detect medical abnormalities, activation level, or recruitment order, or to analyze the biomechanics of human or animal movement.
Medical uses
EMG testing has a variety of clinical and biomedical applications. EMG is used as a diagnostics tool for identifying neuromuscular diseases, or as a research tool for studying kinesiology, and disorders of motor control. EMG signals are sometimes used to guide botulinum toxin or phenol injections into muscles. EMG signals are also used as a control signal for prosthetic devices such as prosthetic hands, arms, and lower limbs.
An acceleromyograph may be used for neuromuscular monitoring in general anesthesia with neuromuscular-blocking drugs, in order to avoid postoperative residual curarization (PORC).
Except in the case of some purely primary myopathic conditions EMG is usually performed with another electrodiagnostic medicine test that measures the conducting function of nerves. This is called nerve conduction studies (NCS). Needle EMG and NCSs are typically indicated when there is pain in the limbs, weakness from spinal nerve compression, or concern about some other neurologic injury or disorder. Spinal nerve injury does not cause neck, mid back pain or low back pain, and for this reason, evidence has not shown EMG or NCS to be helpful in diagnosing causes of axial lumbar pain, thoracic pain, or cervical spine pain. Needle EMG may aid with the diagnosis of nerve compression or injury (such as carpal tunnel syndrome), nerve root injury (such as sciatica), and with other problems of the muscles or nerves. Less common medical conditions include amyotrophic lateral sclerosis, myasthenia gravis, and muscular dystrophy.
Long-term electroencephalographic (EEG) monitoring is the process of recording an EEG for a prolonged period in order to document epileptic seizures or other episodic disturbances of neurologic function. Indications for long-term EEG monitoring include diagnosis of a seizure disorder (epilepsy), classification of seizure types in patients with epilepsy, and localization of the epileptogenic region of the brain. Methods used for long-term EEG monitoring include prolonged analog or digital EEG, prolonged analog or digital ambulatory EEG, and prolonged analog or digital video-EEG monitoring with telemetry. Each of these methods has distinct advantages and disadvantages, particularly relative to storage, retrieval, and manipulation of data. Long-term EEG monitoring is useful in the management of patients with epilepsy and in the diagnosis of a seizure disorder.
Preparing for your Visit
- If you need a referral, please either bring it with you or call your primary doctor and have them send it to us. We cannot see some patients without a referral, confirm with your insurance to see if you need one.
- Bring your photo ID and insurance card.
- Bring your primary doctor’s card or information.
- Think of and write down all of your healthcare related questions to discuss with your doctor during your visit.
- Know your medical history including dates you have been hospitalized or have had surgery, along with any diseases that run in your family.
- If you are taking any medications, be sure to let our doctors know during your time with them along with what doses you are taking.
- Lastly, bring any relevant exams or medical records you may want our doctors to look at.
Plan to arrive 15 minutes before your scheduled appointment for the check-in process.
Wash your hair the night before or the day of the test, but don't use conditioners, hair creams, sprays or styling gels. Hair products can make it harder for the sticky patches that hold the electrodes to adhere to your scalp.
If you have any questions, please call the office and the Medical Assistant will go over instructions and answer your questions.
- Plan to arrive 15 minutes before your scheduled appointment for the check-in process.
- Your appointment with the physician, including the test, will take approximately 45 to 60 minutes. The length of a study varies depending on the condition. Most studies require 30 minutes or less. More involved studies, such as conditions affecting more than one extremity, may take more than an hour.
- Take all of your medications as you normally would.
- Bring or wear loose fitting clothing. For neck and arm studies, it is helpful to wear a sleeveless shirt. For back or leg problems, bring shorts.
- Inform your physician if you take anti-coagulants such as Plavix or Coumadin. You do not need to stop them, but it is important for them to know you are taking them.
If you have any questions, please call the office and the Medical Assistant will go over instructions and answer your questions.
Innovation
Utilizing cutting edge research and equipment to most effectively treat our patients.
Expertise
Over 20 years of experience and training from world-renowned institutions.
Excellence
Ensuring the care you receive is state-of-the-art.